|
5/2/2024 0 Comments Second degree burns definition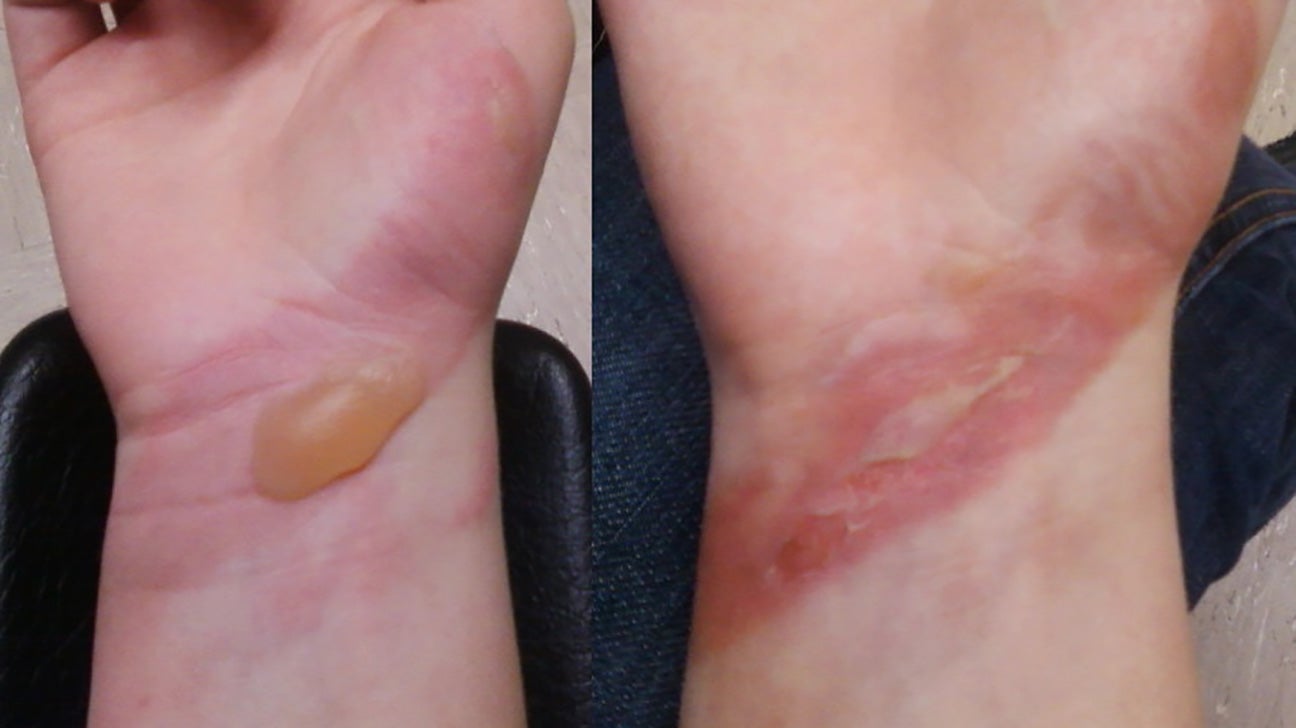
Burns can also occur as a result of self-harm or violence between people (assault). Alcoholism and smoking are other risk factors. In the workplace, risks are associated with fire and chemical and electric burns. In the home, risks are associated with domestic kitchens, including stoves, flames, and hot liquids. Burns occur mainly in the home or the workplace. Most burns are due to heat from hot liquids (called scalding), solids, or fire. Pain medication, intravenous fluids, tetanus toxoid Ī burn is an injury to skin, or other tissues, caused by heat, cold, electricity, chemicals, friction, or ultraviolet radiation (such as sunburn). 
Open cooking fires, unsafe cook stoves, smoking, alcoholism, dangerous work environment Heat, cold, electricity, chemicals, friction, radiation Third degree: Area stiff and not painful įirst degree, Second degree, Third degree, Fourth degree Therefore, medical providers must take the necessary precautions to prevent such complications.Dermatology Critical care medicine, plastic surgery Complications, such as infection, hypertrophic scarring, or contractures, can greatly affect a patient's physical function and mental well-being. 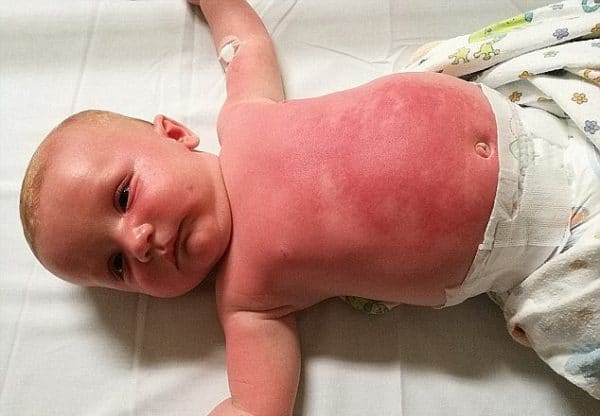
While some burns may heal without intervention, not all can be treated appropriately without surgical intervention. It is crucial for medical providers to accurately evaluate the depth of a burn and be aware of the transfer criteria if the patient is not initially assessed in a certified burn center. Superficial burns are not included in the calculation of TBSA. TBSA can be calculated using various methods, such as the Rule of Nines, the Lund-Browder chart, and the Rule of Palms. Other reasons for transfer include chemical burns, electrical burns, inhalation injuries, and a total body surface area (TBSA) greater than 10%. These criteria include burns that affect the face, hands, feet, genitalia, perineum, and any area with full-thickness burns. The American Burn Association (ABA) has established guidelines that outline 10 criteria for transferring patients to a burn center. Nursing, Allied Health, and Interprofessional Team Interventions These burns take more than 8 weeks to heal and require surgical treatment. The nerves at this depth are also damaged, resulting in the patient experiencing no sensation or pain. At this depth, the affected area does not blanch under pressure due to compromised blood supply. These burns result in a leathery, stiff, and dry appearance. They also extend into the subcutaneous tissue. Ī third-degree burn, also known as a full-thickness burn, is most severe and affects the epidermis and dermis skin layers. Once the blisters are debrided, the underlying wound bed is mottled and will sluggishly blanch with pressure. The patient with a partial-thickness burn experiences minimal pain, which may only be present with deep pressure. These burns can heal without surgery, but it takes longer, and scarring is unavoidable. Similar to superficial partial-thickness burns, these burns can also present with blisters intact. These burns are painful. Healing typically occurs within 2 to 3 weeks with minimal scarring.Ī deep partial-thickness burn involves the deeper reticular dermis. Blisters are common and may still be intact when first evaluated. Once the blister is unroofed, the underlying wound bed is homogeneously red or pink and will blanch with pressure. Ī second-degree burn, also known as a superficial partial-thickness burn, affects the superficial layer of the dermis. Superficial burns heal without scarring within 5 to 10 days. Ī superficial (first-degree) burn involves the epidermis only. These burns can be pink-to-red, without blistering, are dry, and can be moderately painful. The epidermis primarily acts as a protective layer that prevents fluid loss, while the dermis provides skin elasticity and strength. The reticular dermis is more dense and contains more organized elastin, collagen type I and III, and larger blood vessels than the papillary dermis. The papillary dermis is thin and comprises capillaries and various connective tissues like elastin, mainly collagen type III, and reticular fibers. Underneath the epidermis lies the dermis, which consists of the superficial papillary dermis and deep reticular dermis. The outermost layer, the epidermis, contains multiple layers and significant cell components such as melanocytes and keratinocytes. Knowing the skin's structure is crucial in identifying the appropriate burn depth. The skin comprises 2 layers: the epidermis and the dermis. Burn injuries are a complex process and should be documented with a focus on the patient's comorbidities and the injury mechanism. These classify burns into levels based on thickness according to the American Burn Criteria. To accurately determine the depth of a burn, four essential components must be evaluated: appearance, blanching to pressure, pain, and sensation. When categorizing burns, the main factor to consider is depth.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
